My mother’s nursing home kept paper charts for decades. Notes were handwritten, sometimes illegible. Orders were faxed, sometimes lost. Medication lists were updated manually, sometimes missed. When she had an allergic reaction to a newly prescribed drug, no one caught the interaction because no system flagged it. That near-miss finally pushed the facility into the digital age.
Electronic health records are the backbone of modern nursing home tech. Instead of paper charts scattered across different shifts, everything lives in one secure digital system. Medication orders, nursing notes, lab results, therapy progress, all accessible instantly. The first benefit I noticed was legibility. A nurse who can’t read a doctor’s handwriting might give the wrong dose. Digital records eliminated that risk entirely.
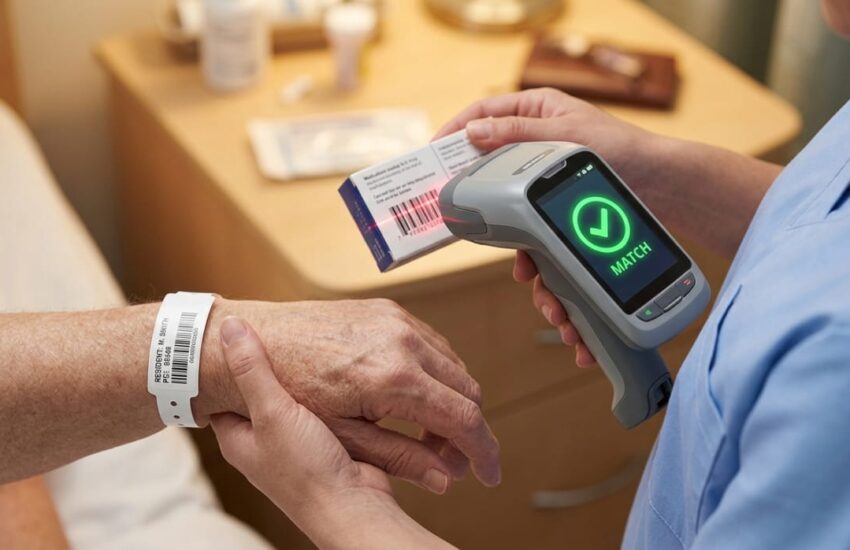
Medication management improved dramatically. The old system relied on nurses checking paper MARs against what was in the cart. Mistakes happened. The new system uses barcode scanning. The nurse scans the resident’s wristband, then scans the medication. If it’s wrong, the system alerts immediately. My mother was nearly given another resident’s blood pressure pill once. The scanner caught it.
Clinical decision support is another game-changer. When a doctor enters an order, the system checks for allergies, drug interactions, and duplicate therapies. It flags inappropriate doses for elderly kidneys. It reminds staff when vaccines or lab tests are due. These automated checks catch errors that human brains miss, especially during night shifts.

Care coordination improved too. Before digital records, the day shift didn’t always know what the night shift had seen. Specialists sent reports by mail. Families got updates only when someone remembered to call. Now everyone works from the same information. The primary care doctor sees what the physical therapist noted. The family can access a secure portal with lab results and daily updates.
Telemedicine became essential during the pandemic, but it’s valuable even now. My mother saw a wound specialist through a video call because driving her to an appointment was exhausting. The specialist examined the wound via high-resolution camera, talked to the nurse on site, and adjusted the treatment plan without my mother ever leaving her bed. That would have been impossible without health IT.
The facility also implemented an electronic fall reporting system. When a resident fell, staff documented it immediately on a tablet. The system aggregated data across the building, identifying patterns. Which hallway had the most falls? What time of day? What medications were involved? The nursing administration used that data to target interventions, more frequent checks during high-risk hours, non-slip mats in problem areas, medication reviews for residents who fell repeatedly.
For families, resident portals were a revelation. I could log in from home and see my mother’s vital signs, upcoming appointments, medication changes, and daily notes from staff. I didn’t have to guess or wait for a call back. That transparency built trust. When I had concerns, I could reference specific data points, not vague impressions.
Not everything was perfect. The transition to digital records was rocky. Staff complained about extra computer time. Some nurses struggled with the new workflows. Older physicians resisted. But within six months, most of the complaints faded. The technology became routine, then essential.
Cost is a real barrier. Small nursing homes struggle to afford these systems. The hardware, software, training, and ongoing support add up quickly. But studies show that health IT reduces adverse drug events, lowers hospital readmission rates, and improves documentation. In the long run, good technology pays for itself.
If you’re evaluating nursing homes, ask about their health information technology. Do they use electronic health records? Barcode medication administration? Telemedicine? A family portal? The answers will tell you whether the facility is investing in safety and quality.
My mother’s facility eventually became a showcase for health IT. But for me, the win was simpler. No more allergic reactions. No more lost orders. No more guessing. The technology didn’t replace human care. Nurses still held hands. Aides still offered comfort. But the technology supported them, caught their errors, and made their good care even better.
There’s so much more to learn about technology and aging. Our website is filled with articles on nursing home quality, safety innovations, and advocating for better care. Head over and explore, because good technology supports good care, and your loved one deserves both.
References
Medicare and Medicaid Policy Analysis Center. (2022). *Health information technology*. In *Nursing home quality: Data and strategies*. National Center for Biotechnology Information. https://www.ncbi.nlm.nih.gov/books/NBK584661/
Pradhan, R., Dayama, N., Morris, M., Elliott, K., & Felix, H. (2024). Enhancing nursing